July 13, 2021
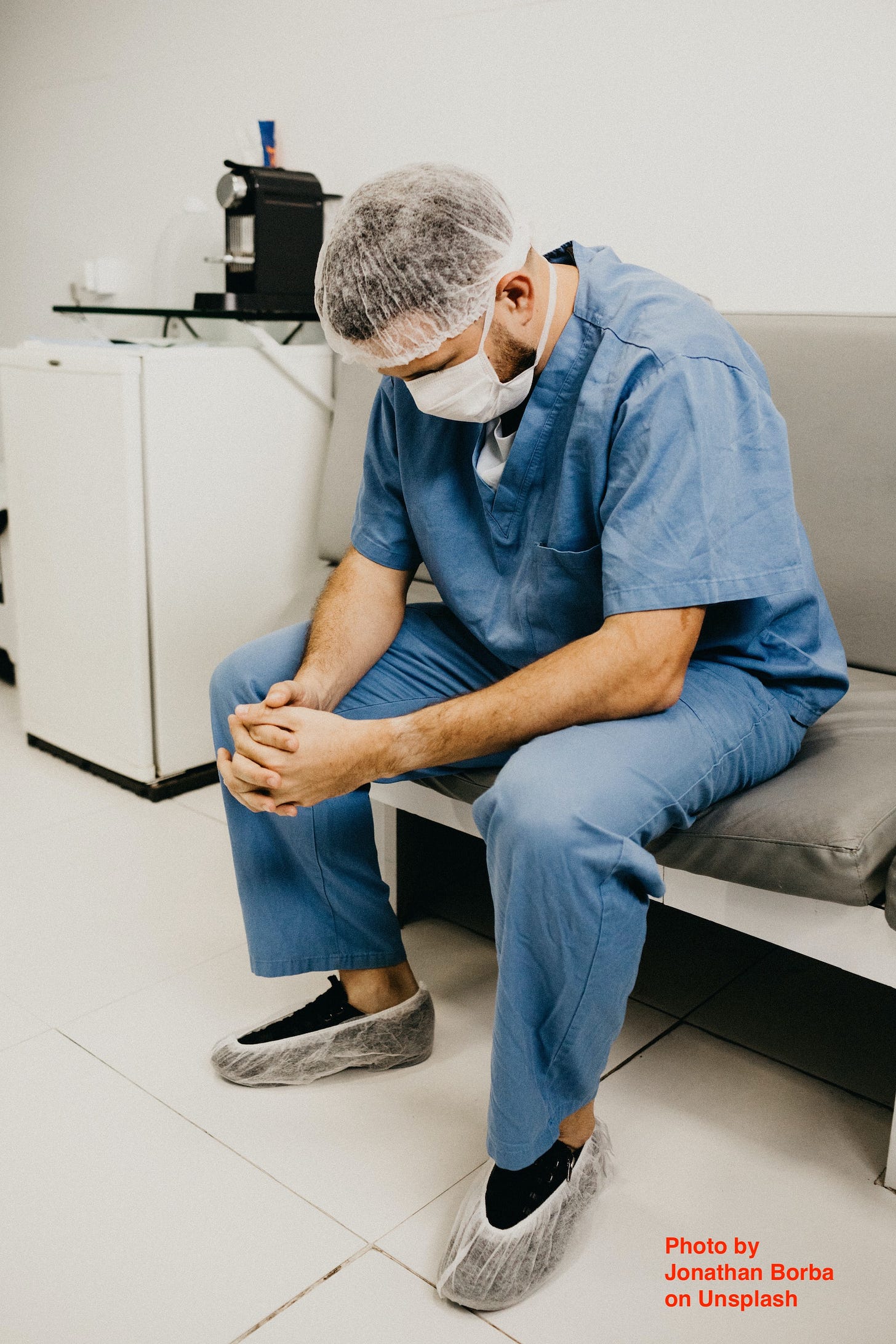
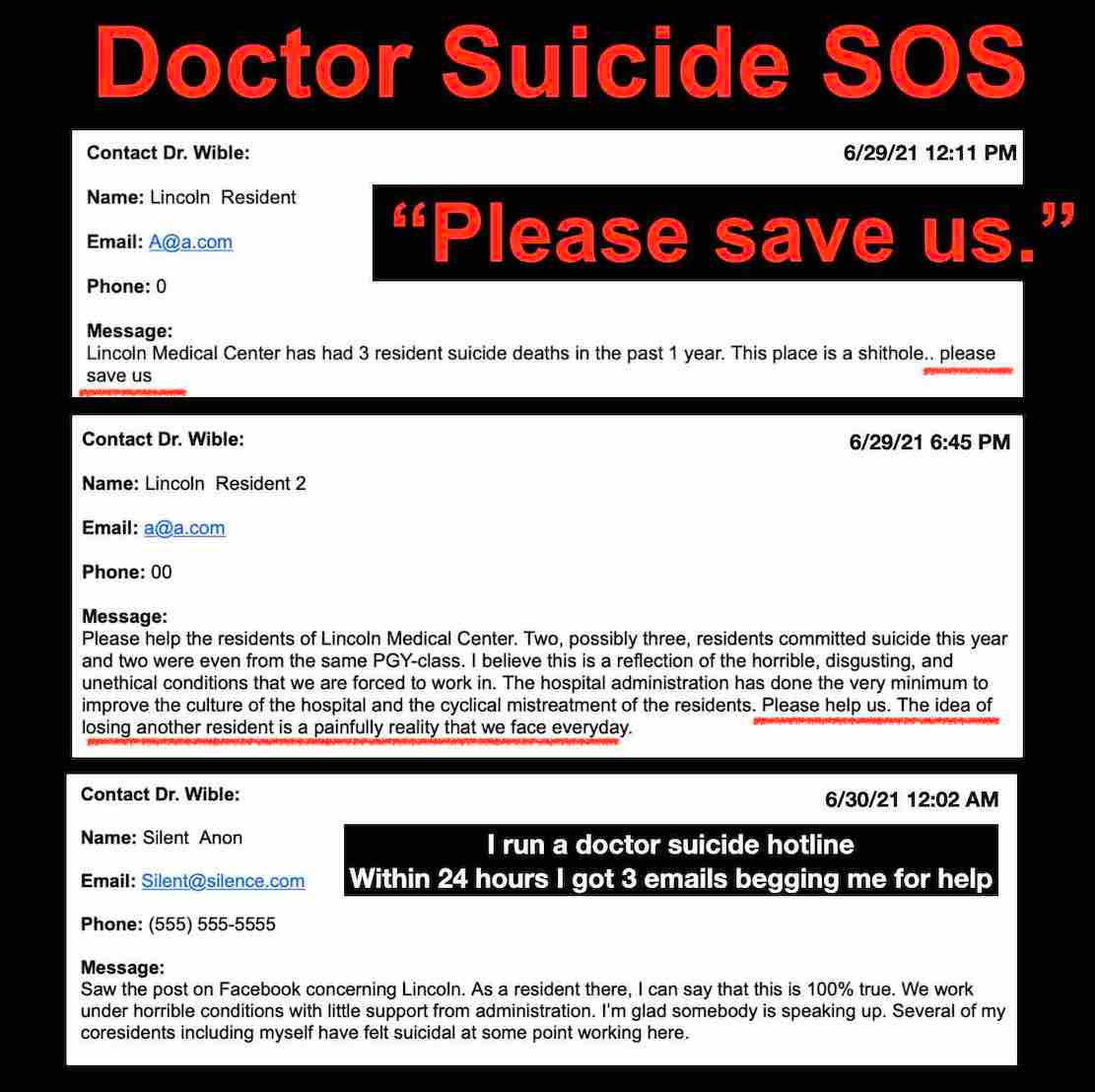
Pamela Wible’s urgent email informs me of another cluster of young physician-in-training suicides. Yes, another cluster in New York.
“Doctor Suicide SOS – ‘Please save us.’ ”
My mind reels, not only from the fact of a doc’s suicide, nor even from the fact of three young physicians driven to an act of desperate finality in one Internal Medicine residency program. It stays stuck in a crazy loop of incomprehension and helplessness that I can’t seem to break out of.
Three residents. In one presumably ACGME-accredited Internal Medicine program. At one presumably Joint Commission-accredited hospital.
In my experience, most non-high-end academic programs have about 20-25 PGYs (post-graduate year, short for residency slots) total for that whole medical or surgical specialty program. About five or six per PGY year for a four-year program. (Residency years are often referred to simply as “PGY[1,2,3…]” designating where you are on the training totem pole. And some smaller institutions may have only one specialty program like Family or Internal Medicine; others may have a fuller gamut including Pediatrics, Obstetrics and Gynecology, General Surgery, and others.
Now presuming my estimate is valid, that’s three of twenty young physicians in an IM program - a 15% suicide mortality incidence in one year.
As we know from the metaphor of the canary in the coal mine, if the canaries that died of hypoxia serve as an indicator, then there’s an entire gradation of PGYs who are likewise hypoxic but not yet dead. This same reasoning applies to the epidemic of burnout. Those who aren’t frankly burned out aren’t necessarily in peak psychosocial fitness. Many are suffering from pre-burnout weardown, much the same way that a sedentary overweight couch potato is a heart attack in waiting.
Where’s the Medical ‘Navy Seal’ Rescue Team?
Now, were this a school camping trip gone disastrous, or a cave exploration trip turned nightmarish, a team of Navy Seals would’ve been sent to rescue the survivors. And there’d be a commission - or several - to examine the excursion’s details, not to allocate blame but to better understand the calamity to see what can be done to prevent such disasters in the future. However, apart from my dear compassionate colleague Dr. Pamela Wible’s heart-rending piece, I don’t know of any medical system alarms going off, any emergency rescue teams storming in to assess this concentrated human disaster and effect remedial rescue operations. Why wouldn’t the state hospital division, or the Dept of Health, or ACGME or the Joint Commission send a team to investigate? Why isn’t the state medical society involved in this? Why isn’t the state medical board, an institution so ardently concerned about protecting patient wellbeing?
Are the Medical Community, Perhaps Society as a Whole, Indifferent?
What’s going on here? Is this such a ho-hum occurrence in American medicine and its training institutions? Is everyone just blasé about it, thinking “Oh well, too bad … I guess they just couldn’t take the pressure.” Given some of the nearly psychopathic comments I’ve seen in various medical forums regarding other physicians’ suicides, I could imagine some (I earnestly hope still a minority) saying “well, it’s good they’re tested now to see if they can take the heat of being a doc because if they can’t, we just as soon know now.” These compassionless physicians, hiding behind the pseudo-tough facade of Spartanism, are almost reflexive in their condemnation of those who allegedly “can’t take the heat” of physicianhood.
I wish I could attribute the lack of compassion-rooted grief to just that select few from the philosophical land of medical Sparta. But as I - with radical honesty here - examine my own unfiltered internal dialog as I process this, I hear myself running a similarly Spartan judgmental dialog. “Too bad,” I hear myself saying, “they probably had a preexisting depression.” And “yep, medical training’s a tough ordeal, and it feels like you’re always in over your head, but …” I’m condescendingly lecturing them, “you’ve got to keep telling yourself that others have survived these wicked currents, and so can you ….”
And then I think to myself, surely no responsible PGY program would be so sadistically boot camp-ish that they wouldn’t attend to their own PGYs’ experiences of drowning, of desperation …. Surely, if as a physician you saw parents of a child acting so negligently toward their safety and wellbeing, you’d advocate for the children to be immediately placed in foster care.
But I immediately catch myself and see how the old tropes grounded in my own training - not such a sweet nostalgia I assure you - persist in contaminating what should be a more objective and less prejudicially biased reflection.
So I sober up my sloppy thinking and more closely examine the stream of verbal effluent that passes as reason.
“They had preexisting depression.” Likely bullshit. But even if they did, the vast majority of people grappling with depression don’t kill themselves. And besides, if you’re able to navigate med school and navigate your concurrent depression, it means your depression didn’t overcome your coping capacity. And further, if your job is driving people to depression and suicidal ideation, then fair to say, there’s a problem with the job.
“Well, it’s good they’re tested before they go into practice.” More insane bullshit. Testing the capacity for endurance is one thing. Pushing to the point of desperation is another.
“Aw, too bad they didn’t have a mentor who could help them buck up and see this as a rough patch.” Another smug privileged prescriptive I’m telling myself. Sure, a benevolent mentor of mythic proportion, a white-cloaked stethoscope-bearing Gandalf of Lord of the Rings would be so helpful. But hoping for such in a desolate place is little more than touchy-feely new-agey fantasizing that makes the advice-giver feel so wise and well-meaning but is completely devoid of reality. It’s really no different than the simplistic directives we offer to the impoverished homeless “well, ya just need to get a job ….”
Confronting Our Indifference That Emanates From Smarmy Snap Judgment
What I’ve not been doing, and I suspect this pertains to so many of us, is confronting my smarmy snap judgment ‘reasoning’ about how things are supposed to be and taking time to look with laser focus at the reality of what exists now. And what exists right now is not pretty.
And it’s difficult to think about, I know. This is not pleasant ‘feel good’ stuff. It’s gory, gloomy, pain-filled. For some of us, it throws us back into our own traumatic training. Who wants to delve into such a downer. Especially given that we each have so much on our plates. But even that rationale doesn’t really stand up to scrutiny. We always have so much on our plates, and much of that has been by choice.
But delve we must. We’ve got to examine what led up to this brutal ending for these three aspiring young physicians. And how is what is going on in THIS program similar to other programs, whether within this institution or at others.
We need to understand this because this current culture in medicine is killing deeply good and talented people. How insane is that!? It would be like telling job applicants to an ER staff position “oh, by the way, three of twenty of our staff kill themselves each year.”
What confluence of factors is going on here that contributes to a mortality rate of 15% - at that by suicide! - of physician trainees in one program? Complex problems are inherently multi-factorial. To simply attribute single causality - at that on an entirely presumed basis - to such a micro-epidemic is as reductionistic as smugly saying that COVID is God’s way of punishing the world for its sinfulness. That God might be greatly disappointed in this sorry lot known as humanity would not be surprising. (Hope there’s a divine therapist s/he can sound it out with. Lordy, the last thing we need right now is a Creator feeling like off’ing himself.)
But these snap-judgment definitive conclusions don’t get us anywhere. In addition to being false and perpetuating flawed stereotypes, they don’t move us toward some actionable understanding.
We must not remain passive, simply shrugging our shoulders in a “too bad but … not my problem” stance. It IS our problem.
The fact is, in this suicide cluster, so far we don't know. But as so many of us tend to do in situations that are outside of our knowledge and immediate relevance domain, we resort to simplistic and judgment-laden causality conclusions.
For example:
“He was depressed.”
“He had an anxiety disorder before starting residency.”
“The attendings there are nasty.”
“The patients are relentlessly abusive.”
“The veteran nurses treat the newbie docs abusively.”
“They were ill-prepared FMGs from second rate med schools.”
“The administration is tyrannical.”
“ It’s a hellhole within a hellhole.”
“They were weak … just couldn’t take the heat.”
They’re all lazy statements of ignorance-based omniscient judgment that we let pass as reason.
Here’s a challenge: take this risky radical self-honesty experiment right now. Blurt out and write down your own take on this suicide calamity and then dare to pause to critically reflect on it.
In this age where snappy tweets have replaced thoughtful reflection, we’re all prone to it. But to address problems like this, we need to examine this newly embedded bad mental habit.
So, how ever do you get to the nexus of causality of such a cluster of suicide mortality? Is it even possible to holistically understand such elusive psychologically-based events?
Yes, it is. In the same way you study physical disease outbreaks or system calamities like the BP Gulf Oil disaster. You do it patiently, deliberately, thoughtfully, thoroughly, objectively, working as an investigative team, together striving to make sense of a complex calamity that has many interrelated causal components.
But before such can take place, you have to have the will to do this. And you have to have the expert resources in place to pursue it and the will to take action on what you’ve learned.
A Psychological Autopsy ?
Little known to many, in the case of suicide, you have a special tool available - the psychological autopsy. Yes, there is such a thing. Just as a board-certified pathologist expertly and systematically performs an autopsy on the physical body, so too a comprehensive postmortem examination can be made of the person’s bio-psycho-social realm. The investigator pours through the complex of factors that seem to have contributed to the coalescence of desperation that led to suicide.
If it is true, as some directly knowledgeable commenters have observed, that that hospital and its PGY IM program is in fact a hellhole of a program within a hellhole of an institution, then that also needs to be taken into consideration as a significant contextual if not driving factor and treated no differently than if the investigator discovered lead paint or radioactive water or bat feces in the hospital basement containing SARS2.
We must not remain passive, simply shrugging our shoulders in a “too bad but … not my problem” stance. It IS our problem.
And while we’re pondering ways to approach this inquiry, we must strive to avoid so readily dismissing this calamity and resorting to our usual snap judgments. We should catch ourselves in the act of dismissal and reflect not just on the fact of each of their deaths and their occurrence as a cluster, but on their altruistic lives and what they yearned for in their careers. We must remind ourselves, these young physicians chose to pursue the rigorous path of preparation for what is universally felt to be one of the highest callings of mankind - that of the profession of medicine whose central value is devotion to the diligent treatment of human disease and injury, the alleviation of suffering, and the commitment to advancing the cause of medical science and fostering the training of other dedicated clinicians.
That’s our oath, and we’ve sought this profession proudly, feeling privileged to use our compassion, and intellect, and skills toward the wellbeing of others, and eager to be part of the healing community.
We Are All in This Healing Profession Together.
Dr. Adhiraj Satija, Dr. Bo Yu and Dr. Waleed Saleh Abuhishmeh, like each one of us who has entered this time-honored profession of healing, deserve to be remembered for their devotion to these ideals. We need to take the time to honor them and to redouble our efforts to ensure that our training institutions, despite their placement in disadvantaged communities and ensnarement in broken systems of care, are models striving for educational and treatment excellence. We are all in this healing profession together, and together it is we who can shape the culture of medicine to be the compassionate care system we so long to be a part of.